As healthcare regulation continues to evolve, the shift from fee for service to pay for performance is increasing at a rapid pace. Healthcare organizations have always been tasked with measuring outcomes, but now the future of their businesses depend on it.
For medical practices, the tedious task of KPI reporting may feel like an impediment to patient care, but this blog will provide practical advice about what’s important to measure and how it facilitates sustainable patient care practices. When framed in this light, it is my hope that healthcare organizations, providers, and staff members will be inspired to move past the initial struggle that comes with change and step boldly towards a management model that tracks, adjusts, and serves like a well-oiled machine.
Dr. Robert S. Kaplan is famous for saying that there are two ways for businesses to make money: “sell more, or spend less.” In “How to Solve the Cost Crisis in Health Care” in the September 2011 Harvard Business Review, Robert Kaplan and Michael Porter argue that improved measurement of outcomes and costs can lead to transformational improvements that will dramatically lower the cost of delivering high-quality healthcare.
Research projects conducted at hospital systems in the U.S. and Europe demonstrate the transformative effect of a new approach that accurately measures costs—at the level of the individual patient with a given medical condition over a full cycle of care—and compares those costs with outcomes. The sheer size of the opportunity to reduce healthcare costs—with no sacrifice in outcomes—is astounding.
In the article, Kaplan and Porter debunk three myths:
- Charges are a good surrogate for provider costs
- Hospital overhead costs are too complex to allocate accurately
- Most healthcare costs are fixed
Instead, the authors propose that the way to create a cost measurement system is to:
- Select the medical condition and/or patient population to be examined
- Define the care delivery value chain
- Develop process maps of each activity and the required resources in patient care delivery
- Obtain time estimates for each process step
- Estimate the cost of supplying each patient care resource
- Compute the total costs over each patient’s cycle of care
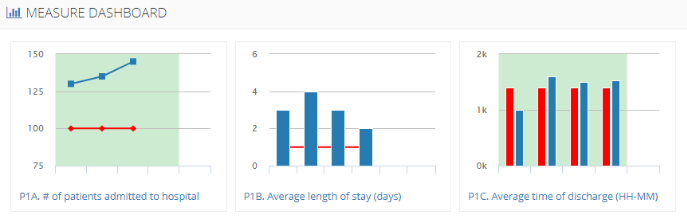
Identifying costs in this way enable healthcare practices to proactively anticipate and respond to patient needs. It is uncertainty that leads to chaos and can leave staff members’ heads spinning. The decomposition of the cost measurement structure not only provides a consistent path forward, but also allows for innovation. Are all of these steps necessary? Are there opportunities to provide better patient care for less? Where can we save time without sacrificing quality? How can we better support our patients as they face the next step in their clinical journey? Answers to these questions lead to improved outcomes for patients and practices.
For more information on how to leverage the Balanced Scorecard and KPI reporting for your healthcare organization, talk to an ESM expert today or check out our BSC resources for healthcare.








